For many moderate to severe dry eye patients, symptoms are manageable at first, then progressively worsen. The process may be gradual or sudden. The research community, despite its ongoing work, has not yet identified the primary “mechanism of action” for many cases of severe dry eye.
This unpredictability raises a dire predicament for patients who rely on self-care remedies to mitigate symptoms. Fortunately, physicians have developed more aggressive treatment methods for severe cases.
In this article, we’ll provide an overview of the five most common therapies and procedures for moderate to severe dry eye patients. Though our views are not intended to replace the advice of your physician, we hope this article gives you a good place to start.
Punctal Plugs (Punctal Occlusion Surgery)
Your tears are always being produced and always being drained. Drainage of the tears occurs through four small drains (the “puncta”). You have a puncta on each upper lid and a puncta on each lower lid. If you are not producing enough tears (or if they are evaporating too fast), these puncta can be plugged (much like plugging a drain) allowing for increased tear retention.
Punctal plugs are an advanced dry eye treatment that blocks the eyes’ tear drainage system by inserting devices called “punctal plugs” into the tear ducts or “puncta.” The procedure aims to preserve natural tears on the surface of the eye.1
Quick Facts
- For patients with moderate to severe dry eye syndrome
- Non-surgical assistance for tear deficiency
- In-office procedure
Benefits of Punctal Plugs
Punctal plugs come in different sizes and are made from different materials, from collagen to silicone.1
Collagen plugs are inserted first. Over the course of 4–7 days, if the procedure shows signs of success, silicone plugs can be inserted for long-term treatment.1
In most cases, the puncta on the lower lid are occluded, and in advanced cases, both the upper and lower lid puncta are occluded.
How To Know If Punctal Plugs Are Right For You
Punctal plugs are a non-surgical procedure, but dilation of the puncta to allow insertion can be uncomfortable, so topical anesthesia is usually used. You should feel pressure, but no pain with topical anesthesia.
In inflammatory dry eyes, there is some concern that inflammatory chemicals and particles will not drain from the ocular surface properly with the use of plugs. Much like a backed up sink, if these substances accumulate, irritation and inflammation can actually increase — negating many of the benefits of tear retention.
Of course, we recommend that you consult with your doctor to discuss the pros and cons of punctal occlusion therapy.
Autologous Serum (AS) Eye Drops
Autologous Serum (AS) Eye Drops are a highly-effective – but costly – alternative to artificial tears.
In a complex process, this “autologous serum” is created from a blood sample supplied by the patient. The result is an eye drop which is a near carbon copy of the patient’s natural tears.2
Quick Facts
- Specialized lubricant for ocular health
- Costly and lengthy formulation process
- Not covered by most health insurance (No FDA approval)
Benefits of Autologous Serum (AS) Eye Drops
Artificial tears and other over-the-counter remedies help lubricate and ease symptoms, but they do not contain the vitamins, proteins, lipids, and growth factors necessary for eye health.
Autologous serum eye drops, meanwhile, carry biological nutrients found in natural tears that are critical to the maintenance of the tear film.3 As eye drops also help to fight inflammation, ensuring patient comfort.4
Scleral Contact Lenses
Scleral lenses are specially-designed contact lenses for patients recovering from corneal damage, as well as for patients suffering from severe dry eye syndrome.
Quick Facts
- For patients with severe dry eye or corneal damage
- Custom-fit to a patient’s eyes for comfort
- May cost up to $4,000 for fitting and lenses
Benefits of Scleral Lenses
More studies examining scleral lenses and dry eye syndrome are needed. Still, researchers have called scleral lenses, “a viable option for severe dry eye syndrome,” that “improve visual acuity and relief of symptoms.”5
Standard contact lenses may contribute to dry eye symptoms, or due to dryness, require that dry eye patients take special care to remove them safely.
Eyelid Thermal Pulsation Technology
Eyelid thermal pulsation therapy relies on a unique device that simultaneously applies heat (thermal) and pressure (pulsation) to open and express the clogged glands.
Quick Facts
- Applies heat and pressure to relieve symptoms of MGD
- FDA-approved & non-invasive
- Short, 12-minute procedure6
Once the hardened meibum is softened and removed, meibomian glands are then free to produce a healthy layer of oil and lipids, preventing tear evaporation.
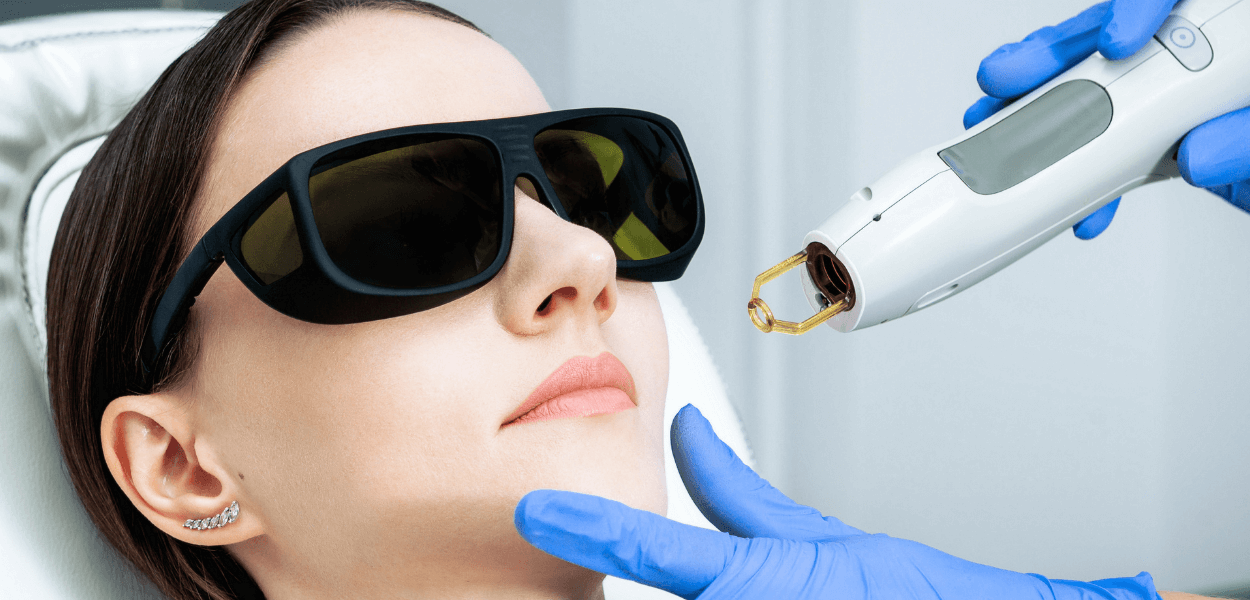
Intense Pulsed Light (IPL) Therapy
Intense Pulsed Light Therapy, or IPL, is a well-documented and effective procedure for symptoms related to meibomian gland dysfunction.
IPL works by directing a controlled spectrum of light to close the blood vessels that supply the glands in the eyelids, stimulating healthy gland function.7
Quick Facts
- In-office procedure
- For evaporative dry eye (meibomian gland dysfunction)
- A safe and effective treatment for rosacea
Benefits of Intense Pulsed Light (IPL) Therapy
IPL decreases inflammation in the eyelids and ocular surface and promotes the production of healthy lipids that block tear evaporation.8
Over the last five or so years, IPL has become a go-to procedure for people suffering from chronic dry eye caused by meibomian gland dysfunction. In one study from the Mayo Clinic, 89% of patients who tried IPL saw improved dry eye symptoms.7
Four Lifestyle Changes For Healthier Eyes
- If the air in your home is dry, try a humidifier. Avoid ceiling fans, and certainly don’t sleep with a ceiling fan on.
- Move your car’s AC vents so that they blow away from your face.
- Use sunglasses outdoors, and make sure the lenses are large enough to cover your eyes.
- Take breaks when reading or using your computer or phone. Try for at least a 20-second break after every 20 minutes looking at a screen.9
References
- Ervin AM, Law A, Pucker AD. Punctal occlusion for dry eye syndrome: summary of a Cochrane systematic review. Br J Ophthalmol. 2019;103(3):301-306. doi:10.1136/bjophthalmol-2018-313267
2. Tsubota K, Goto E, Fujita H, et al. Treatment of dry eye by autologous serum application in Sjögren’s syndrome. Br J Ophthalmol. 1999;83(4):390-395. doi:10.1002/14651858.CD013559
3. Pan Q, Angelina A, Marrone M, Stark WJ, Akpek EK. Autologous serum eye drops for dry eye. Cochrane Database Syst Rev. 2017;2(2):CD009327. Published 2017 Feb 28. doi:10.1002/14651858.CD009327.pub3
4. Semeraro F, Forbice E, Braga O, Bova A, Di Salvatore A, Azzolini C. Evaluation of the efficacy of 50% autologous serum eye drops in different ocular surface pathologies. Biomed Res Int. 2014;2014:826970. doi:10.1155/2014/826970
5. Bavinger, J & DeLoss, Karen & Mian, Shahzad. (2015). Scleral lens use in dry eye syndrome. Current opinion in ophthalmology. 26. 319-324. 10.1097/ICU.0000000000000171.
6. Godin MR, Stinnett SS, Gupta PK. Outcomes of Thermal Pulsation Treatment for Dry Eye Syndrome in Patients With Sjogren Disease. Cornea. 2018;37(9):1155-1158. doi:10.1097/ICO.0000000000001621
7. Intense Pulsed Light for Treatment of Dry Eye Disease. Mayo Clinic. https://www.mayoclinic.org/medical-professionals/ophthalmology/news/intense-pulsed-light-for-treatment-of-dry-eye-disease/mac-20430229
8. Suwal A, Hao JL, Zhou DD, Liu XF, Suwal R, Lu CW. Use of Intense Pulsed Light to Mitigate Meibomian Gland Dysfunction for Dry Eye Disease. Int J Med Sci. 2020;17(10):1385-1392. Published 2020 Jun 1. doi:10.7150/ijms.44288
9. Sheppard AL, Wolffsohn JS. Digital eye strain: prevalence, measurement and amelioration. BMJ Open Ophthalmol. 2018;3(1):e000146.
